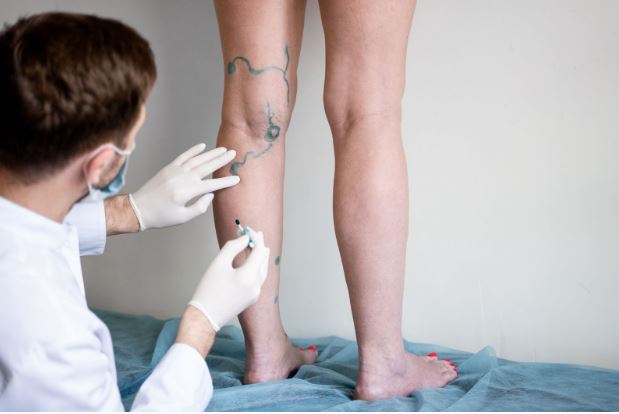
Vein health is one of those areas where people tend to wait too long before seeking help. What starts as occasional leg heaviness or a few visible spider veins can quietly progress into chronic venous insufficiency, skin damage, or open wounds that are genuinely difficult to treat. Knowing when to consult a vascular specialist rather than managing symptoms at home indefinitely is the kind of knowledge that can prevent a manageable condition from becoming a serious one. Heres a practical guide to reading your symptoms at each stage.
Early Warning Signs: What to Watch For
The early symptoms of venous insufficiency are easy to dismiss because theyre common and non-specific. But they follow a recognizable pattern that distinguishes venous issues from ordinary fatigue.
Leg heaviness and aching that worsens through the day, particularly by evening, is one of the most consistent early indicators. This isnt the muscle fatigue youd expect after exercise; its a persistent, pressure-like sensation that results from blood pooling in the veins due to valves that arent closing properly. Some patients describe it as a "lead-like" feeling in the lower legs. Burning and itching often accompany it.
Swelling in the feet and ankles that appears during the day but isnt present in the morning is another characteristic sign. This edema reflects fluid accumulation from elevated venous pressure. Compression stockings can control it temporarily, but if swelling returns consistently, the underlying cause needs assessment rather than indefinite management with compression alone.
Nighttime leg cramps and restless leg symptoms are frequently connected to venous congestion, though this link is often overlooked. If youre being woken regularly by leg cramps or an uncontrollable urge to move your legs, venous insufficiency is worth ruling out.
Visible varicose or spider veins are the most obvious early sign, and the one most often written off as purely cosmetic. While some varicose veins are cosmetic, theyre frequently part of a broader pattern of superficial venous system stress that benefits from proper evaluation.
None of these symptoms individually requires an emergency appointment, but a pattern of several of them — especially if theyve been present for months — is a reasonable prompt for a baseline vascular assessment.
Higher-Priority Symptoms That Need Prompt Attention
As venous disease advances, symptoms shift from subjective discomfort to objective physical changes that indicate tissue damage is beginning. These require timely evaluation from a specialist, not continued home management.
Hemosiderin staining is one of the clearest clinical indicators of progressing chronic venous insufficiency. It appears as reddish-brown or rust-colored patches on the skin near the ankles, caused by red blood cells leaking from the veins into surrounding tissue and leaving iron deposits as they break down. These patches dont respond to topical creams — they reflect whats happening in the veins beneath the skin.
Lipodermatosclerosis is a more advanced skin change involving inflammation, hardening, and tightening of the skin and subcutaneous tissue in the lower leg. The skin may feel hard, leathery, or painful to the touch. In more advanced presentations, the leg takes on an inverted shape — wider above the ankle, narrowed below — that reflects chronic tissue constriction. This requires specialist evaluation and typically indicates that conservative management alone is no longer sufficient.
Venous leg ulcers are open wounds, usually on the inner leg just above the ankle, that develop when tissue damage from prolonged venous hypertension reaches the point of breakdown. These are a significant escalation in severity. Specialist referral is strongly recommended if an ulcer doesnt reduce in size by 25 percent within a month of standard wound care, persists beyond three months, is larger than 10 square centimeters, or appears rapidly without improvement. Untreated venous ulcers dont typically resolve on their own — they require the underlying venous problem to be addressed.
Localized vein tenderness, redness, or warmth may indicate superficial thrombophlebitis, inflammation from a clot just below the skin surface. While distinct from deep vein clots, it warrants medical evaluation to confirm the clot isnt extending into the deep venous system.
Symptoms That Require Emergency Care
Some vascular symptoms dont warrant a scheduled appointment — they require same-day emergency evaluation.
Sudden swelling and pain in one leg — particularly when one leg is markedly more swollen than the other — is a hallmark presentation of Deep Vein Thrombosis (DVT). DVT is a blood clot in a deep vein that can have serious consequences if left untreated.
Shortness of breath, chest pain, or rapid heart rate following leg pain or swelling may indicate a Pulmonary Embolism — a clot that has broken free and traveled to the lungs. This is a life-threatening emergency requiring immediate attention.
Bleeding from a varicose vein can be more significant than it appears because varicose veins are under elevated pressure. If a thinned area of skin overlying a vein ruptures, the bleeding can be difficult to control. Apply firm, continuous pressure and seek emergency care.
Signs of wound infection — spreading redness, warmth, and swelling around an existing wound — may indicate cellulitis, a bacterial skin infection requiring antibiotic treatment. Venous ulcers in particular are vulnerable to infection. If a chronic wound begins showing atypical features — abnormal bleeding, excessive tissue overgrowth, or complete failure to heal despite appropriate care — it requires urgent specialist evaluation to rule out malignant transformation.
Who Should Seek Early Consultation
Certain patient profiles warrant earlier specialist evaluation, before symptoms become severe, because the risk of rapid progression or poor outcomes is higher.
A history of DVT or pulmonary embolism significantly increases the risk of post-thrombotic syndrome, a form of chronic venous insufficiency that can develop after a clot episode. Anyone with this history should be monitored proactively rather than waiting for symptoms to prompt a visit.
Obesity and advanced age are associated with elevated venous pressure and slower healing, both factors that can accelerate the progression from early symptoms to ulceration. Occupational exposure matters too: jobs requiring prolonged standing or prolonged sitting (particularly without regular calf muscle movement) contribute to venous hypertension over time.
Diabetes and chronic kidney disease require careful specialist consideration. Diabetic neuropathy can reduce or eliminate the pain signals that would normally prompt someone to seek care, meaning significant vein disease can develop without the usual warning of discomfort. These patients also face higher risk of concurrent arterial disease, which changes how compression therapy should be applied and makes diagnostic testing essential before treatment begins.
What a Vascular Consultation Actually Involves
A specialist consultation for venous disease is more comprehensive than many patients expect, and the diagnostic tools available make it possible to identify the exact source of the problem before any treatment is planned.
Duplex ultrasound is the primary diagnostic tool — a non-invasive imaging test that visualizes vein anatomy, maps blood flow, and identifies valvular reflux (backward blood flow where it shouldnt occur) or obstructions in both superficial and deep veins. Its the gold standard for pinpointing venous failure and guides all subsequent treatment decisions.
Ankle-Brachial Index (ABI) testing measures the ratio of blood pressure at the ankle to blood pressure at the arm, screening for peripheral artery disease before compression therapy is prescribed. As the Society for Vascular Surgerys clinical practice guidelines outline, identifying arterial insufficiency before applying compression is essential — compression therapy thats appropriate for pure venous disease can cause harm in patients with significant arterial compromise.
Treatment planning follows the diagnostic findings. Many patients begin with compression and lifestyle modifications, but when superficial venous reflux is confirmed, minimally invasive interventions, endovenous ablation or sclerotherapy, have been shown to accelerate healing and reduce recurrence rates compared to compression alone. The consultation should end with a clear, individualized plan rather than a generic recommendation to "keep wearing compression stockings."
The most important thing to understand about venous disease is that it progresses predictably, and intervention at earlier stages produces better outcomes with less complexity than intervention after tissue damage has accumulated. If youre recognizing the early warning signs, a baseline evaluation is the right next step.
下一則: Translating Academic Achievement into Career Readiness: The Role of SCLA
- How to Prepare for Your First Driving School Appointment
- Medicare Advantage Enrollment Dates and Deadlines 2027: A Clear Guide to Timing, Coverage Changes, and Important Medicare Windows
- Comprobación de Aislamiento 10 kV y Prueba de Capacidad de Baterías en Sistemas Eléctricos
- Midnight Shutdown: When Repairs Turn Into a Fire Risk
- The Ultimate Resource for Finding Professional Fire Watch Companies
- Why Your Business Needs Quality Colorado Mountain Modern Furniture
限會員,要發表迴響,請先登入


